In a hospital, ambulance or a remote village in sub-Saharan Africa, researchers are focused on improving pregnancy outcomes with access to high-quality obstetric ultrasound, when and where it’s needed.
Each year some 300,000 women and 3 million babies worldwide die during childbirth or shortly thereafter, according to the World Health Organization, which recommends ultrasound for all pregnancies before 24 weeks’ gestation. However, in many settings, as few as 5% of pregnant women receive any ultrasound care.
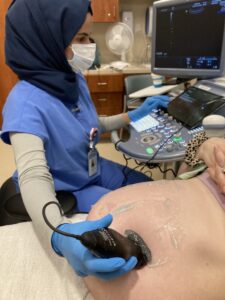
Researchers at Carolina funded by the Bill & Melinda Gates Foundation are working on a solution.
Last spring, in a landmark UNC study, the team of researchers proved fetal gestational age can be achieved using an artificial intelligence (AI) prediction tool with a low-cost, battery-powered diagnostic probe connected to a smartphone.The novel ultrasound model outperformed expert sonographers in Zambia and Chapel Hill.
Now, the researchers have received a third round of funding to develop 10 tools that will make the benefits of ultrasound available almost anywhere, including North Carolina.
The work demonstrates the mutually beneficial nature of global health research that can improve the delivery of health care services both abroad and close to home.
Led by Dr. Jeff Stringer, professor of obstetrics and gynecology and associate director of the UNC Institute for Global Health and Infectious Diseases, this interdisciplinary research team from the School of Medicine, Gillings School of Global Public Health (GSGPH) and Institute for Global Health and Infectious Diseases, is working to improve pregnancy outcomes using technologies to expand obstetrical ultrasound access in low-resource settings. Their work offers hope to millions of pregnant women when it comes to determining risks and sequencing optimal care.
“Our work foretells a future where all pregnant women, not just those who live in wealthier countries, will be able to access the diagnostic benefits of obstetric ultrasound,” said Stringer.
Jumping the hurdles and pushing down the barriers.
Dr. Stringer came up with the idea for the study when he and his wife Elizabeth worked as obstetricians in Lusaka, Zambia.
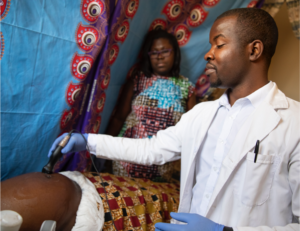
“Ultrasound is like a stethoscope to the modern obstetrician, used to determine gestational age, evaluate growth and development, and in some cases, evaluate possible problems or confirm a diagnosis,” said Dr. Stringer. “The gold standard is to have a qualified, trained sonographer perform an ultrasound using a standard cart-based machine, and a doctor to interpret it.”
But in low-resource settings like Zambia, which is typical of care systems across sub-Saharan Africa and parts of Asia, the high cost for equipment and the need for trained sonographers to perform scans means that very few women have access to ultrasound.
In contrast, more than 12 million scans are performed each year in the U.S., with the average pregnant woman receiving three to four ultrasounds during pregnancy, or more, for complicated pregnancies.
Yet, in rural areas of the U.S., including parts of North Carolina, women may face lengthy travel to access obstetric care. As trauma centers have closed, so have obstetric units. North Carolina ranks number three in rural hospital closures, a situation that worsened during the pandemic by delaying nonessential services that bring in revenue. For pregnant women, this could mean more births outside of hospitals, births in hospitals without OB care, and preterm births–all of which carry greater risks for a mom and baby.
Conducting the study in Zambia and North Carolina
From September 2018 through June 2021, 4,695 pregnant volunteers in North Carolina and Zambia received blind ultrasound sweeps of the abdomen alongside standard fetal measurements collected on both the commercial ultrasound machine and a low-cost, battery-powered device (Butterfly iQ).

Three test data sets were used to assess the performance of the AI model and standard measurements against previously established gestational age.
Michael Kosorok, PhD, GSPGH Professor of Biostatistics, and his lab, collaborated to create and train a neural network that could estimate gestational age from the sweeps. Joint first authors Teeranan (Ben) Pokaprakarn, PhD, and Juan C. Prieto, PhD, led deep learning training, data analysis and creative problem solving.
Joni Price, MD, MPH, UNC Assistant Professor of Obstetrics and Gynecology, who lives full time in Zambia and led study implementation at the Lusaka site, says the study has the potential to revolutionize obstetric care.
“Armed with a pocket-sized probe and a smartphone, a midwife with no prior training in sonography can assess gestational age as accurately as a certified sonographer using an expensive machine.”

In the next study phase, researchers will develop and validate other AI-enabled low-cost ultrasound devices while collecting data to support widespread recommendation and adoption by agencies like WHO and national Ministries of Health.
Dr. Stringer says the research team embraces the opportunity to advance technology that can help pregnant women everywhere in the world.
“We teach trainees that what we learn as researchers and what we deliver to patients in any community has global implications. We are never isolated in our approach to health.”
